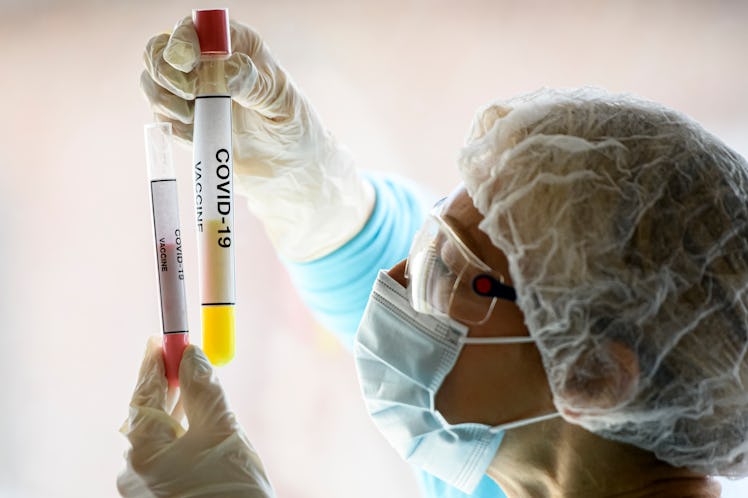
Here's What To Know About When You Might Get A Coronavirus Vaccine
If you're looking forward to a world without COVID-19, here's some good news. After months of breakneck development and rapid clinical trials, several major pharmaceutical companies, including Moderna, Pfizer, and AstraZenica, have succeeded in generating highly effective vaccines against the novel coronavirus. However, as the U.S. continues to face fallout from the virus on all possible fronts, scientists predict the pandemic will get worse before the Food and Drug Administration (FDA) approves a treatment. This begs the question: When will a coronavirus vaccine be available to the public? There's a light at the end of the tunnel.
According to a report from the Centers for Disease Control and Prevention (CDC), once approved for an emergency use authorization, the COVID-19 vaccine should be available before the end of 2020 — with some shipments coming in as soon as mid-December. However, these preliminary shipments only carry a limited supply, and the treatment won't be immediately available to everyone.
Who can expect to receive the vaccine first? According to Peter Palese, Ph.D, chair of the Microbiology Department at Mt Sinai's Icahn School of Medicine, it's highly likely long-term care patients, the elderly, and those with underlying conditions will be top priority. "It's a very difficult decision for health officials to make, but it's critical for high-risk individuals to receive treatment as soon as possible," Palese states, noting how health care workers, first responders, and essential workers are also prioritized groups.
Young adults in good health (like most college students) are decidedly lower on the list of urgency, since the virus is much less likely to prove fatal for them. "College students already think they're immortal," Palese jokes. But it's kind of real. "For the most part, that's true when it comes to this virus. When you're that age, your body is more well-equipped to handle sickness than someone older who's of higher risk." However, both Palese and the CDC emphasize that everyone should follow proper health and safety guidelines by socially distancing, wearing a mask, and minimizing their risk factor by getting their yearly flu-shot. As supplies for the treatment increase over time, all adults should have access to the vaccine in 2021. "If distribution is handled effectively, we can expect things to get much better very soon," Palese states.
The vaccine is coming after nearly a year of missteps and challenges and an enormous death toll. As of Dec. 4, the ongoing coronavirus pandemic has claimed the lives of over 276,000 Americans, per The New York Times. Daily fatality levels have officially reached an all-time high, with the U.S. topping over 3,157 deaths in a single day on Nov. 2 — effectively shattering death records set during the early stages of the pandemic in the spring.
During those critical early stages, the federal government failed to release strategies for nation-wide testing, and instructed states to buy their own emergency medical equipment to cope with the virus, such as respirator masks, drugs, ventilators, goggles, gloves, and more. In cities with large populations, such as New York and Chicago, hospitals were so ill-equipped to handle the heightened COVID-19 death toll that they had to use makeshift morgues to hold dead bodies.
In a Nov. 12 report from APM Research Lab, researchers found that "Black, Indigenous and Latino Americans all have a COVID-19 death rate of triple or more White Americans, who experience the lowest age-adjusted rates." Per the CDC, contributing factors to these disproportionate death rates include the lack of health care access and utilization, the presence of educational, income, and wealth gaps, as well as discrimination in occupation and housing. As the vaccine is rolled out, experts are considering how to make sure it's distributed equitably along racial, ethnic, and economic lines.
"Because of the pandemic, we're able to see inequities within our communities that were already present much more clearly now," said Rupali J. Limaye, Ph.D, MPH, MA, the director of Behavioral and Implementation Science at Johns Hopkins University's International Vaccine Access Center, during a media event on Dec. 3. She noted it will be critical for the United States to make a concerted effort to reach low-income, high-risk communities that may have "less access to health care in general, and consequently, less access to the vaccine."
This is why, per Palese, it's absolutely imperative for the treatment to be handled as a public good that is accessible and affordable to everyone in America. "These are extremely desperate times, and the pandemic has negatively affected the health and financial security of millions of people across the country," Palese tells Elite Daily. "This vaccine should be available to all, without regard to social standing or financial capabilities."
The first shipments of the vaccine from Pfizer, which carry a 95% efficacy rate, are expected to arrive in the U.S. as soon as Dec. 15, per CNN.
If you think you’re showing symptoms of coronavirus, which include fever, shortness of breath, and cough, call your doctor before going to get tested. If you’re anxious about the virus’s spread in your community, visit the CDC for up-to-date information and resources, or seek out mental health support. You can find all Elite Daily's coverage of coronavirus here.
Experts Cited:
Peter Palese, Ph.D, Horace W. Goldsmith Professor and chair of the Microbiology Department at Mount Sinai's Icahn School of Medicine
Rupali J. Limaye, Ph.D, MPH, MA, the director of Behavioral and Implementation Science at Johns Hopkins University's International Vaccine Access Center