7 Questions You Should Ask Yourself Before Getting An IUD
Dating as a millennial woman is often fraught with difficulty.
While the idea of dating should be fun, more often than not, the realities of dating aren't great. On top of the bad seeds we're forced to sift through on Tinder and Bumble, sometimes including a sea of secretly married men and unwarranted dick pics, women are also forced to deal with the idea of an unwanted pregnancy that may come from a sexual encounter.
Luckily, it's 2017 and our options are more expansive than just relying on a man to put a condom on properly.
Although many women default to oral hormonal birth control (also known as "The Pill"), intrauterine devices, or IUDs, are becoming more mainstream.
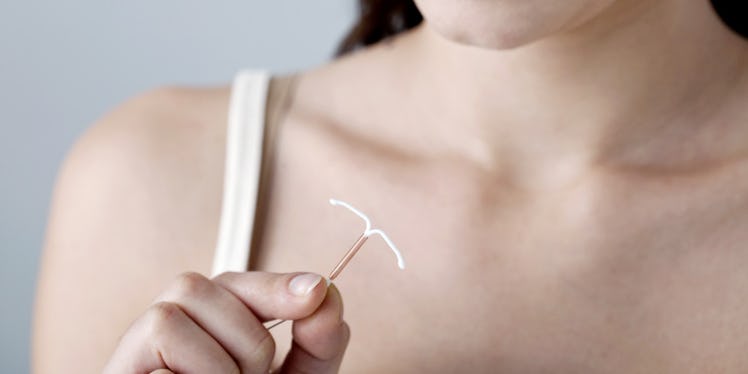
An IUD is a small device, shaped like the letter "T," that goes inside a woman's uterus to prevent pregnancy. This procedure is done in a medical office and from there, the IUD stays put for three to 10 years until it's taken out.
If a daily pill isn't your jam, an IUD may be a good choice for you. Also, if you aren't into hormones, a copper IUD, as opposed to a hormonal one, could be just the ticket.
I had a copper IUD for seven years before I had my tubes tied (I'm in the "I never want and/or wanted kids" camp), but I only found out about IUDs as an option because I'm related to an OBGYN. My own physician never gave me the info on IUDs, nor had I really found much information on them myself. When I realized it was an option, I was thrilled: It involved no hormones, no daily pill, and a high rate of effectiveness.
But how do you know if an IUD may be for you?
Elite Daily spoke to some experts in order to help form questions to ask before deciding to go and get an IUD.
1. Just how effective is an IUD?
According to Planned Parenthood, IUDs are some of the most effective means of birth control available now. In fact, they're more than 99 percent effective. Planned Parenthood's website states:
IUDs are so effective because there's no chance of making a mistake. You can't forget to take it (like the pill), or use it incorrectly (like condoms). And you're protected from pregnancy 24/7 for three to 12 years, depending on which kind you get. Once your IUD is in place, you can pretty much forget about it until it expires.
Dr. Jennifer Caudle, Family Physician, and Assistant Professor at Rowan University School of Osteopathic Medicine, says, "[M]ost women are able to use an IUD, and they are very effective. According to the American Congress of Obstetricians and Gynecologists (ACOG) the IUD is one of the most effective forms of reversible birth control. Less than one in 100 women using an IUD will become pregnant in the first year of use."
2. Which IUD should I get?
There are two primary types of IUDs: copper and hormonal.
I had the copper IUD, known as ParaGard, for several years, and I chose it specifically because it was hormone-free. When I got it, I was told it was effective up to 10 years, but the FDA has since updated its use for up to 12 years.
The five hormonal IUDs available (that are FDA approved in the U.S.) are Mirena, Kyleena, Skyla, and Liletta. Hormonal IUDs use progestin, which is similar to the natural hormone progesterone, to prevent pregnancy. According to Planned Parenthood, Mirena works for up to six years, Kyleena for up to five, and Skyla and Liletta for up to three years.
If you aren't into hormones and want longer-term protection, ParaGard might be right for you. If you don't mind the additional hormones and wouldn't mind taking your IUD out a bit sooner, any of the hormonal methods could also work.
3. How much pain is involved in getting an IUD?
IUDs aren't the most comfortable to put in.
I was advised to take ibuprofen before my appointment and then to take more later in the day. I won't lie to you: It wasn't fun... and I was feeling pretty miserable the rest of the day. From what I have researched however, my level of pain wasn't common.
Everyone's situation is different. Most women will only feel a small amount of pain (or even just some mild discomfort) when the IUD is getting put in. You might have a doctor that uses a numbing treatment or you might feel a bit dizzy after - it really depends on you.
Just be aware that it won't be the most pleasant procedure in the world.
4. How much does an IUD cost?
This answer can vary, with IUDs ranging from zero dollars under insurance to hundreds of dollars out-of-pocket.
Luckily, a lot of health plans can help cover IUDs. The cost generally includes the exam or exams leading up to the insertion, the insertion, and any needed follow-ups.
You can also check with your local Planned Parenthood on options to get a free or low-cost IUD, or you may be eligible to receive one through another government program.
Though an IUD might cost more upfront, in the long-term, you wouldn't be taking a daily pill or other on-going methods of birth control so it will likely end up costing less overall.
5. Do IUDs protect against STIs?
Be aware that IUDs only protect against unwanted pregnancy.
You'll still need to find a way to protect yourself against STIs.
For this, condoms are still the best options, along with regular health screenings. You can also use foams, creams or jelly to help protect against STIs, although they tend to be less favored than condoms.
6. Can an IUD be used as an emergency contraception?
ParaGard is the most effective form of emergency contraception available today. Having a ParaGard inserted within five days of unprotected sex has an over 99 percent effectiveness.
That said, just like "Plan B" or "the morning-after pill," it's never a good idea to rely on emergency contraception as your primary method of birth control.
Planning to prevent pregnancy before it happens is your best bet, instead of frantically figuring out how to prevent it after the fact.
7. What are some other things to know before getting an IUD?
Some general positives of IUDs include that once you put it in, you never have to think about it again.
Also, it's totally reversible! Fertility often comes back more quickly post-removal compared to the Pill. In fact, you can normally get pregnant again as soon as your IUD is out.
As far as some negatives, the IUD does require some not-so-fun moments during the insertion and of course, it doesn't protect you from STIs. Some women may not be able to use it at all, like those allergic to copper or those that have difficult with progestin.
There is also a small chance (about five percent) of the IUD falling out and an even small chance (about 0.01 percent) of the IUD perforating your uterus (which, very rarely, has to be corrected with surgery).
IUDs can be a great option for those looking for something outside of the Pill or condoms. Kristin Marie Bennion, a licensed Mental Health Therapist and Certified Sex Therapist, says she's seen an increase in clients bringing up the topic of IUDs, which she says "has seemed to correlate with fears that women may soon lose access to reproductive health care."
Bennion added,
Since a large portion of women prefer the use of oral contraceptives, which requires a monthly prescription, the loss of healthcare can make an IUD can [offering pregnancy prevention for up to 10 years in some cases] begin to sound rather appealing.
To assess whether an IUD may be right for you, speak up and chat with your healthcare provider.
There's no rule that oral birth control has to be your only option to prevent pregnancy.